 
Vision will be counting fingers or worse day 1 in the presence of intraocular gas, which can be particularly unnerving for patients who had good vision preoperatively, such as those with macula-on detachments. The patient’s retina surgeon should have prescribed a postoperative regimen of drops consisting of a topical broad-spectrum antibiotic and a steroid for 1 week, followed by a weekly taper of the steroid. EARLY POSTOPERATIVE PERIODĪ standard postoperative schedule should generally involve visits at days 1 and 7, and one visit between weeks 3 and 4. Perfluorocarbon in the anterior chamber of an eye viewed through a slit lamp. Although perfluorocarbon is not intended to stay within the eye for an extended period, as it will lead to inflammation, silicone oil is frequently left inside the eye to prevent further detachments.įigure 2. Other materials, such as silicone oil and perfluorocarbon (Figure 2), are used in situations of chronic inferior detachments, repeat detachments, or in the presence of proliferative vitreoretinopathy. An air bubble in the vitreous will last 4 to 5 days, whereas SF 6 can last up to 2 weeks and C 3F 8 can last between 8 and 12 weeks. Over time, these bubbles are reabsorbed safely into the body, as the vitreous cavity fills with aqueous humor. The exact composition of the gas varies from surgeon to surgeon but is usually a mixture of either SF 6 plus air or C 3F 8 plus air. Although PPV for floaters or vitreous hemorrhage may require air-fluid exchange (in which the vitreous cavity is filled with sterile saline), a retinal detachment or macular hole generally requires a tamponade with gas to eliminate trans-hole fluid flow, thus restoring the transretinal pressure gradient required to keep the retina attached. Once the retina is reattached, or the membrane is peeled, etc., the vitreous cavity may be filled with any number of materials, including gas, liquid, and oil (the type of material chosen depends on the procedure performed). Macula-off retinal detachment before (A) and after (B) PPV. This ensures that further manipulation within the globe is less likely to cause iatrogenic retinal breaks through inadvertent vitreous traction.įigure 1. Every surgery, whether for primary rhegmatogenous retinal detachments (RRDs), intraocular foreign bodies, or another retina condition, begins with the generalized removal of the vitreous (Figure 1). These incisions are performed through the pars plana, hence the term pars plana vitrectomy (PPV). Three points of entry into the eye, called sclerotomies, enable the surgeon to illuminate the retina while performing the vitrectomy. A vitrectomy is usually performed under monitored local anesthesia and can take anywhere from 15 minutes to more than 2 hours, depending on the pathology and complexity of the case. 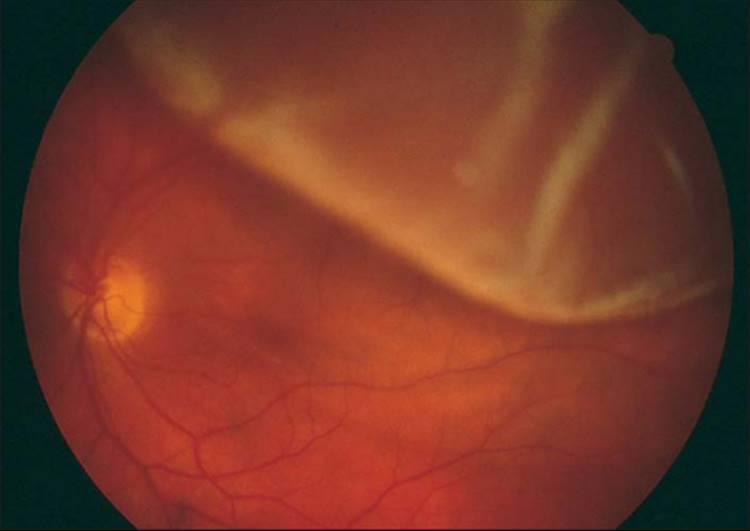
The term vitrectomy means the surgical removal of the vitreous, which is typically accomplished with a vitrector (a small, specialized tool that cuts the vitreous into small segments before removing them from the eye). This article examines the role we can play in comanaging our patients in the days and weeks following a vitrectomy. Thanks to recent advances in techniques and technology, modern day, small-gauge vitrectomy has revolutionized retina surgery, providing a faster, less invasive, often sutureless procedure for a variety of vitreoretinal pathologies. Optometrists provide excellent postoperative management for a variety of ocular procedures. Identifying the etiology of the pain is important. High IOP may be caused by expanding gas or a steroid response. Low IOP at postoperative day 1 requires close inspection of the sclerotomies for possible leakage.A standard postoperative schedule should generally involve visits at days 1 and 7 and one visit between weeks 3 and 4. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
